The global dialysis machines market is experiencing robust growth, driven by the rising prevalence of chronic kidney disease (CKD), an aging population, and increased healthcare expenditure. According to Mordor Intelligence, the dialysis equipment market was valued at USD 16.5 billion in 2023 and is projected to grow at a CAGR of over 6.8% from 2024 to 2029. Similarly, Grand View Research estimates the global dialysis devices market to reach USD 24.3 billion by 2030, expanding at a CAGR of 6.7% from 2023. This sustained demand has intensified competition among manufacturers to innovate in efficiency, patient comfort, and automation. As the industry evolves, a select group of leading companies are shaping the future of renal care through advanced technology and global outreach. Here, we highlight the top 8 dialysis machine manufacturers leading this transformation.
Top 8 Dialysis Machine Manufacturers 2026
(Ranked by Factory Capability & Trust Score)
#1 A New Way of Experiencing Dialysis
Domain Est. 2014
Website: outsetmedical.com
Key Highlights: Tablo is a simple, versatile approach to reducing the cost and complexity of dialysis. Learn more. Top of the Tablo machine. All-in-one technology ……
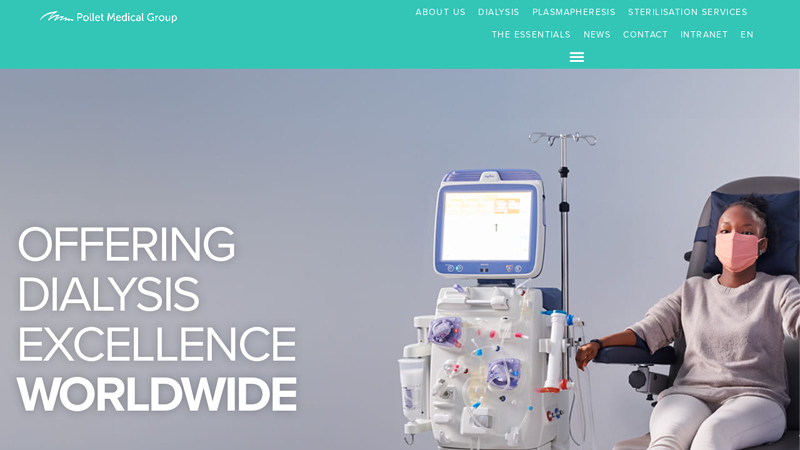
#2 Worldwide
Domain Est. 2019
Website: polletmedicalgroup.com
Key Highlights: Farmasol is a dialysis XPRT and manufacturer of Hemodialysis products. As one of the few companies, Farmasol produces almost all hemodialysis consumables ……
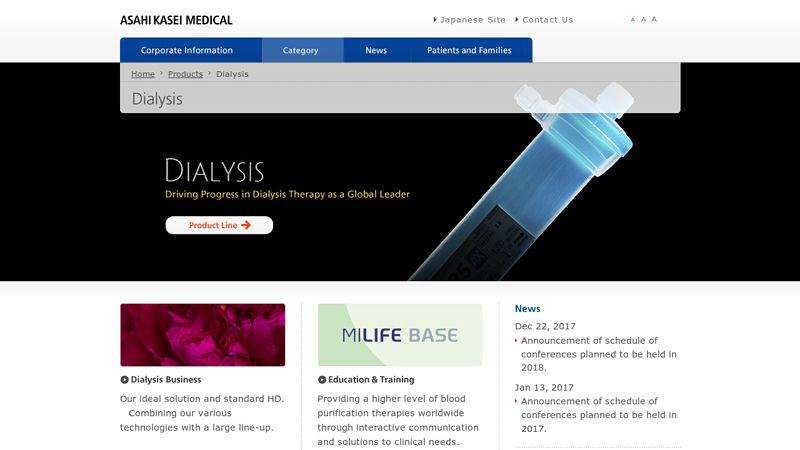
#3 Dialysis
Website: asahi-kasei.co.jp
Key Highlights: Dialysis products – We offer high-performance dialyzers that improve therapeutic effectiveness and contribute to patients’ quality of life….
#4
Domain Est. 1995
Website: fresenius.com
Key Highlights: We save and improve human lives with affordable, accessible, and innovative healthcare products and the highest quality in clinical care….
#5 Fresenius Kabi Global Website
Domain Est. 1998
Website: fresenius-kabi.com
Key Highlights: Fresenius Kabi stands for integrity, human rights, and ethical business, building trust through transparency, compliance, and responsible global supply chains….
#6 Machines overview
Domain Est. 2000
Website: freseniusmedicalcare.com
Key Highlights: Hemodialysis machines and devices. Fresenius Medical Care 6008 CAREsystem and 5008S CorDiax machines enable HighVolumeHDF as a standard in dialysis. The ……
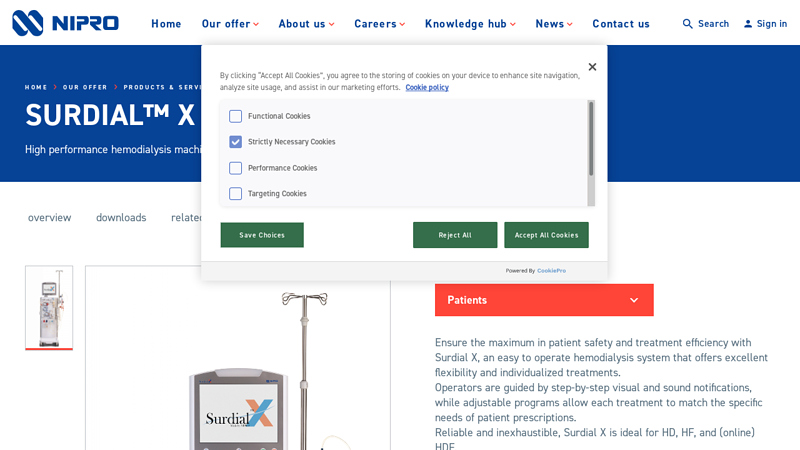
#7 Surdial™ X
Domain Est. 2008
Website: nipro-group.com
Key Highlights: Surdial™ X is a high performance hemodialysis machine designed for individually optimized treatments, offering excellent flexibility and personalized care….
#8 SWS dialysis,medical,sws hemodialysis machine,CRRT,dialyzer
Domain Est. 2024
Website: swsdialysis.com
Key Highlights: Its branded products include:SWS dialysis,SWS medical,SWS dialysis machine,SWS hemodialysis … The official website of SWS company is:www.swsdialysis.com….
Expert Sourcing Insights for Dialysis Machine

2026 Market Trends for Dialysis Machines
The global dialysis machine market is poised for significant transformation by 2026, driven by demographic shifts, technological innovation, healthcare policy changes, and increasing prevalence of chronic kidney disease (CKD). This analysis explores key trends shaping the dialysis machine landscape in the coming years.
Rising Prevalence of Chronic Kidney Disease
One of the primary drivers of the dialysis machine market is the escalating global burden of chronic kidney disease. According to the Global Burden of Disease Study, over 850 million people worldwide suffer from some form of kidney disease—a number expected to rise due to increasing rates of diabetes, hypertension, and aging populations. By 2026, the International Society of Nephrology projects that the number of patients requiring dialysis will exceed 5 million, creating robust demand for dialysis machines across both developed and emerging markets.
Technological Advancements and Innovation
By 2026, the integration of digital technologies into dialysis machines is expected to redefine patient care. Key innovations include:
- Smart Dialysis Machines: Devices equipped with AI-driven analytics, remote monitoring, and predictive maintenance are gaining traction. These machines can adjust treatment parameters in real time, improving patient outcomes and reducing complications.
- Portable and Home-Based Systems: There is a growing shift toward home hemodialysis (HHD) and peritoneal dialysis (PD), fueled by patient demand for convenience and cost pressures on healthcare systems. Compact, user-friendly machines such as the NxStage System One and new entrants from companies like Medtronic and Baxter are expanding access to home care.
- Wearable and Implantable Devices: Though still in developmental stages, wearable artificial kidneys (WAKs) are expected to enter late-stage clinical trials by 2026, potentially revolutionizing long-term dialysis therapy.
Market Expansion in Emerging Economies
Developing regions—particularly in Asia-Pacific, Latin America, and Sub-Saharan Africa—are expected to witness the fastest market growth. Countries like India, China, and Brazil are investing in healthcare infrastructure and expanding insurance coverage for dialysis treatment. Government initiatives and public-private partnerships are increasing dialysis machine availability in rural and underserved areas. By 2026, the Asia-Pacific region is forecasted to account for over 35% of global market growth.
Regulatory and Reimbursement Landscape
Regulatory approvals and reimbursement policies will heavily influence market dynamics. In the U.S., the Centers for Medicare & Medicaid Services (CMS) continue to refine payment models under the End-Stage Renal Disease (ESRD) Prospective Payment System, incentivizing cost-effective and high-quality care. Similarly, the European Union’s Medical Device Regulation (MDR) is pushing manufacturers to enhance device safety and clinical evidence, affecting time-to-market for new products. Favorable reimbursement policies in countries like Japan and South Korea are also accelerating adoption of advanced dialysis systems.
Competitive Landscape and Strategic Moves
The dialysis machine market remains dominated by key players such as Fresenius Medical Care, Baxter International, B. Braun, and Asahi Kasei. However, increased competition from regional manufacturers and startups focusing on digital health and home dialysis is reshaping the industry. Strategic partnerships, mergers, and R&D investments are expected to intensify by 2026, particularly in areas like tele-nephrology integration and AI-powered diagnostics.
Sustainability and Cost Pressures
Healthcare systems worldwide are under pressure to reduce the cost of dialysis, which remains one of the most expensive chronic care treatments. This is driving demand for reusable components, energy-efficient machines, and preventive care models aimed at delaying CKD progression. Additionally, sustainability concerns are prompting manufacturers to explore eco-friendly materials and reduce the environmental footprint of dialysis operations.
Conclusion
By 2026, the dialysis machine market will be characterized by technological sophistication, geographic diversification, and a strong emphasis on patient-centric care. The convergence of innovation, policy support, and unmet clinical needs presents significant opportunities for stakeholders across the nephrology ecosystem. As home-based and smart dialysis solutions become mainstream, the industry is moving toward a future where dialysis is not only more accessible but also more personalized and efficient.

Common Pitfalls in Sourcing Dialysis Machines: Quality and Intellectual Property (IP) Risks
Sourcing dialysis machines, critical medical devices for patients with kidney failure, involves significant responsibilities. Overlooking key quality and intellectual property (IP) aspects can lead to severe consequences, including compromised patient safety, regulatory non-compliance, financial losses, and reputational damage. Here are common pitfalls to avoid:
Inadequate Quality Assurance and Regulatory Compliance Checks
One of the most critical mistakes is failing to thoroughly verify the quality and regulatory standing of the dialysis machine and its manufacturer. Key pitfalls include:
- Neglecting Regulatory Approvals: Sourcing machines without confirming valid regulatory approvals (e.g., FDA 510(k) or PMA in the US, CE Marking in Europe, local country approvals) is a major red flag. Machines lacking proper certification cannot be legally sold or used clinically in most jurisdictions.
- Overlooking ISO 13485 Certification: Failing to ensure the manufacturer holds current ISO 13485 certification (Quality Management System for medical devices) indicates a lack of standardized processes for design, production, and quality control, increasing the risk of defects.
- Insufficient Verification of Manufacturing Standards: Not verifying adherence to essential safety and performance standards (e.g., IEC 60601 series for electrical safety, ISO 15223 for labeling) can result in machines that are unsafe for patients and healthcare providers.
- Inadequate Due Diligence on Supplier Track Record: Ignoring the manufacturer’s history of recalls, safety alerts, or regulatory actions can lead to sourcing unreliable equipment. A poor track record often signals underlying quality management issues.
- Compromising on Component Quality: Assuming all components (tubes, filters, sensors) meet required specifications without verification. Substandard components can lead to treatment failures, infections, or machine downtime.
Intellectual Property (IP) Infringement and Counterfeit Risks
Sourcing dialysis machines, especially from unfamiliar suppliers or secondary markets, carries significant IP-related dangers:
- Procuring Counterfeit or Refurbished-as-New Devices: Acquiring machines that are outright counterfeits, or refurbished units misrepresented as new. This poses severe safety risks due to unknown history, potential component degradation, and lack of warranty. Counterfeits often bypass rigorous quality controls.
- Sourcing from Unauthorized Distributors: Purchasing through channels not authorized by the original equipment manufacturer (OEM). This increases the risk of receiving non-genuine products, voided warranties, and lack of access to OEM technical support or software updates.
- Infringing on Patents or Design Rights: Unknowingly sourcing machines that incorporate patented technologies (e.g., specific blood pumping mechanisms, monitoring algorithms, user interface designs) without proper licensing. This can lead to costly legal disputes, injunctions, and financial penalties for both the buyer and seller.
- Using Unauthorized Software or Firmware: Installing or using software modifications, cracks, or pirated firmware to bypass features or extend functionality violates software copyrights and licensing agreements. This compromises device safety, security, and regulatory compliance.
- Ignoring Trademark Violations: Acquiring machines with altered or counterfeit branding/logos, which is not only illegal but also indicative of a lack of quality control and traceability.
Mitigation Strategies
To avoid these pitfalls, implement rigorous sourcing protocols:
- Prioritize Authorized Channels: Source directly from OEMs or their officially authorized distributors.
- Demand Documentation: Require proof of regulatory approvals, ISO 13485 certification, and genuine product origin.
- Conduct Supplier Audits: Perform on-site or third-party audits of manufacturers, especially for high-value or long-term contracts.
- Verify Serial Numbers: Check device serial numbers against OEM databases to confirm authenticity and warranty status.
- Engage Legal and Compliance Teams: Involve experts to review contracts, IP clauses, and regulatory compliance aspects before finalizing purchases.
- Establish Clear Contracts: Include warranties, service agreements, IP indemnification clauses, and clear definitions of new vs. refurbished equipment.
By proactively addressing these quality and IP pitfalls, healthcare providers and procurement organizations can ensure the safe, reliable, and legally compliant acquisition of dialysis machines, ultimately protecting patient welfare and organizational integrity.

Logistics & Compliance Guide for Dialysis Machines
Overview
Dialysis machines are critical medical devices used in the treatment of patients with kidney failure. Due to their life-sustaining function, stringent logistics and compliance protocols must be followed during transportation, installation, operation, and maintenance. This guide outlines key considerations to ensure safe, compliant, and efficient handling of dialysis machines across the supply chain and clinical settings.
Regulatory Compliance
Dialysis machines are classified as Class II or Class III medical devices under most regulatory frameworks, requiring adherence to strict standards.
– FDA (U.S.): Must comply with 21 CFR Parts 800–898, including registration, listing, Quality System Regulation (QSR), and adherence to premarket notification (510(k)) or approval (PMA) requirements.
– EU MDR (European Union): Requires CE marking under Regulation (EU) 2017/745. Manufacturers and importers must ensure conformity assessment, technical documentation, and post-market surveillance.
– Other Regions: Compliance with local regulations such as Health Canada (Medical Devices Regulations), Japan’s PMDA (PMD Act), and Australia’s TGA (Therapeutic Goods Act) is mandatory.
– Standards: Adherence to ISO 13485 (Quality Management), ISO 14971 (Risk Management), and IEC 60601-1 (Electrical Safety) is essential.
Transportation & Handling
Proper logistics are vital to prevent damage and ensure device integrity.
– Packaging: Machines must be shipped in manufacturer-approved, shock-resistant packaging with humidity and temperature indicators.
– Environmental Controls: Transport should maintain temperatures between 10°C and 40°C and avoid excessive humidity or vibration. Climate-controlled vehicles are recommended.
– Labeling: Packages must display “Fragile,” “This Side Up,” and medical device identifiers. Include UN3481 labels if lithium batteries are included.
– Handling Procedures: Use trained personnel and appropriate equipment (e.g., pallet jacks) to prevent physical damage. Avoid tilting beyond manufacturer specifications.
Import & Customs Clearance
International shipments require thorough documentation and regulatory checks.
– Required Documents: Commercial invoice, packing list, bill of lading/airway bill, Certificate of Conformity, FDA 510(k) or CE Certificate, and import license (if applicable).
– Customs Classification: Use correct HS Code (e.g., 9018.90 for medical instruments) to determine duties and restrictions.
– Licensing: Some countries require import permits or pre-approval from health authorities (e.g., ANVISA in Brazil, SFDA in Saudi Arabia).
– Duty & Tax Exemptions: Explore eligibility for humanitarian or medical device duty exemptions where applicable.
Storage & Inventory Management
Post-delivery storage must protect device integrity.
– Storage Conditions: Keep in a clean, dry, temperature-controlled environment (15–30°C, 30–70% RH). Avoid direct sunlight and corrosive agents.
– Inventory Tracking: Implement barcode or RFID systems to monitor expiration of accessories (e.g., tubing, filters) and service intervals.
– Security: Restrict access to authorized personnel only; maintain audit trails for high-value medical equipment.
Installation & Commissioning
Installation must follow manufacturer and regulatory protocols.
– Site Preparation: Ensure adequate power supply (voltage, grounding), water quality (for hemodialysis machines), and space per manufacturer guidelines.
– Qualified Personnel: Installation and calibration must be performed by trained biomedical engineers or manufacturer-certified technicians.
– Documentation: Complete installation checklists, maintain service logs, and update asset management systems.
Maintenance & Servicing
Routine maintenance ensures safety, performance, and regulatory compliance.
– Scheduled Servicing: Follow manufacturer-recommended intervals (e.g., monthly, quarterly) for preventive maintenance.
– Calibration & Testing: Perform electrical safety checks, hydraulic tests, and alarm verifications as per IEC 62353.
– Service Records: Maintain detailed logs, including parts replaced, software updates, and technician certifications. Required for audits and inspections.
Training & Operator Certification
Only trained personnel should operate dialysis machines.
– Initial Training: Provide comprehensive instruction on setup, operation, emergency procedures, and infection control.
– Competency Assessment: Document staff training and conduct periodic evaluations.
– Manufacturer Training: Utilize OEM-provided programs to ensure up-to-date knowledge on new features or software.
Post-Market Surveillance & Incident Reporting
Proactive monitoring is required to ensure ongoing safety.
– Adverse Event Reporting: Report malfunctions, injuries, or deaths to relevant authorities (e.g., FDA MedWatch, EUDAMED) within mandated timeframes.
– Field Safety Notices: Distribute and document receipt of any recalls or safety alerts issued by the manufacturer.
– Data Collection: Monitor performance metrics and user feedback to identify potential risks.
Decommissioning & Disposal
End-of-life management must comply with environmental and health regulations.
– Data Wiping: Remove all patient and operational data from machine memory in accordance with HIPAA or GDPR.
– Decontamination: Follow CDC and manufacturer guidelines to disinfect equipment prior to decommissioning.
– Recycling/Disposal: Partner with certified e-waste handlers. Comply with local hazardous waste regulations, especially for batteries and electronic components.
Conclusion
Effective logistics and compliance management for dialysis machines ensures patient safety, regulatory adherence, and operational continuity. Stakeholders—including manufacturers, distributors, healthcare facilities, and regulators—must collaborate to uphold standards throughout the device lifecycle. Regular audits, staff training, and documentation are critical components of a successful compliance program.
Conclusion: Sourcing Dialysis Machine Manufacturers
Sourcing dialysis machine manufacturers requires a strategic and thorough approach, considering the critical nature of these medical devices in patient care. After evaluating various global suppliers, it is evident that key factors such as regulatory compliance (FDA, CE, ISO certifications), product quality, technological innovation, after-sales service, and cost-efficiency play a pivotal role in the selection process.
Leading manufacturers from regions such as North America, Europe, and Asia offer a range of options, from high-end automated systems to cost-effective models suitable for emerging markets. Established companies like Fresenius Medical Care, Baxter International, and B. Braun dominate the market with comprehensive solutions, while emerging players from China and India are gaining traction through competitive pricing and improved quality standards.
For healthcare providers, dialysis centers, or distributors, the optimal choice depends on specific needs—whether prioritizing advanced features, reliability, service network, or affordability. Conducting due diligence, including factory audits, reference checks, and product trials, is highly recommended before finalizing partnerships.
Ultimately, partnering with a reputable and compliant manufacturer ensures not only the delivery of safe and effective dialysis equipment but also supports long-term operational success and improved patient outcomes. Continuous monitoring of market trends and regulatory updates will further aid in making informed sourcing decisions in the evolving landscape of renal care technology.